PHOTO ACTIVATED PLATELET RICH PLASMA
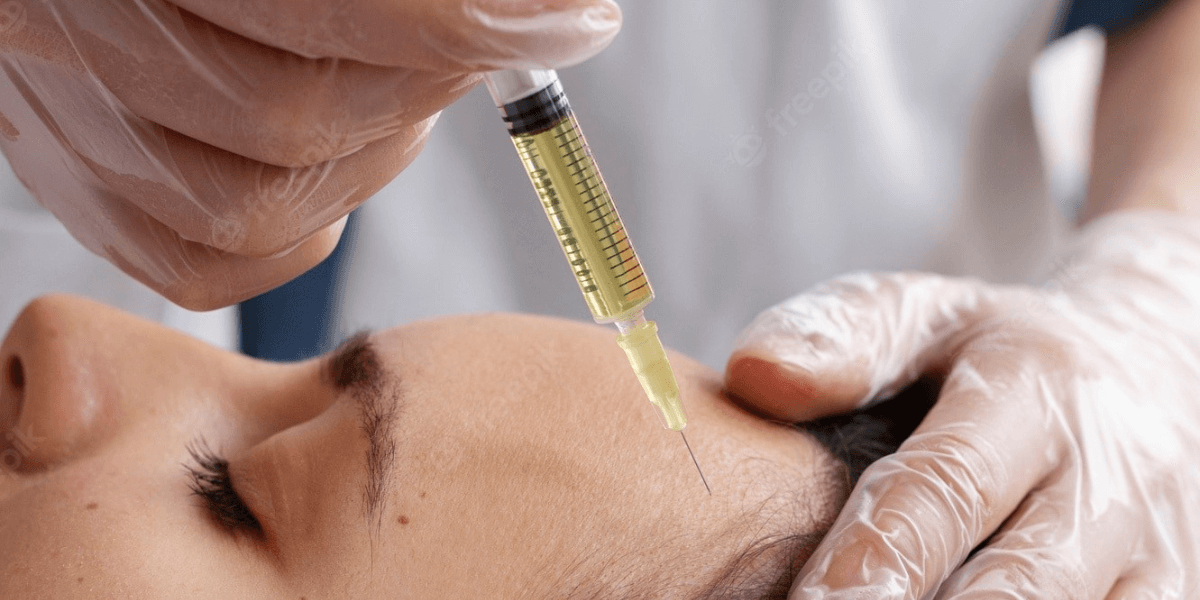
PA-PRP : Platelet Rich Plasma are photo activation before injection back into the patient. For photo activation low intensity light at specific frequencies are uses.
Photo activation of PRP increase the secretion of various inflammatory and healing agents from peripheral blood cells and platelet into PRP Photo activation seems to increase the secretion of tiny vesicles (exosomes) from peripheral white blood cells, stem cells and platelets. Photo activation raises IL-1 Receptor antagonist in PRP.
PRP for musculoskeletal conditions
Platelet-rich plasma, commonly referred to as PRP, is an autologous blood derivative- it is human blood that is spun down and separated, producing a concentration of platelets above normal values. Platelets are the clotting cells of our blood, but they also have great potential in enhancing healing of muscle, tendon and ligaments. Studies suggest that growth factors released by platelets recruit reparative cells, augmenting tissue repair and accelerating soft tissue healing.
What does the process of PRP involve?
After assessing you, a nurse will take your blood (like a standard blood test), which will be spun in a centrifuge to isolate the plasma component.
-Platelet-Rich Plasma (PRP) is activated under a light. Then the PRP is injected directly into the site of injury. The process will take around 45 to one hour.
-Local anaesthetic is injected 15-20 minutes before or at the same time with PRP injection depending on the injury.
How does PRP work?
The growth factors and platelets in the plasma promote cells to multiply and form new tissue, accelerating and enhancing the healing process.
PRP contains a much higher concentration of platelets than normal blood. This means that higher concentrations of growth factors are being released into the injured area.
When compared to cortisone injections, PRP injections hold better results and last much longer. While the effects of cortisone are rapid, they are often followed by a decline in condition. PRP shows slower but greater long-term improvement and less injury recurrence.
What can be treated with PRP?
- Osteoarthritis
- Muscle, ligament, and tendon injuries (including tennis or golfer’s elbow)
- Degenerative knee conditions
- Bursitis
- Cosmetic (hair, face)
- Rotator cuff
- Gynaecological conditions
Growth Factor
PDGF (Platelet Derived Growth Factor)Cell growth, differentiation, blood vessel growth
| Growth Factor | Function |
|---|---|
| TGF-β (Transforming Growth Factor-beta) | Blood vessel, collagen synthesis |
| VEGF (Vascular Endothelial Growth Factor) | Cell growth, migration, and new blood vessel growth |
| FGF (Fibroblast Growth Factor) | Collagen synthesis, blood vessel growth |
| EGF (Endothelial Growth Factor) | New blood vessel growth, cell growth |
| IGF (Insulinlike Growth Factor) | Collagen synthesis with PDGF, cell growth, and differentiation |
PRP Also Contain
- Anti-inflammatory and anti microbial mediators
- IL-1 Receptor antagonist
- Thymosin beta 4-TNF blocker
- Microbiocidal Peptides
- Phospholipade A2
- Serotonin
- Thromboxane A2
- Adenosine